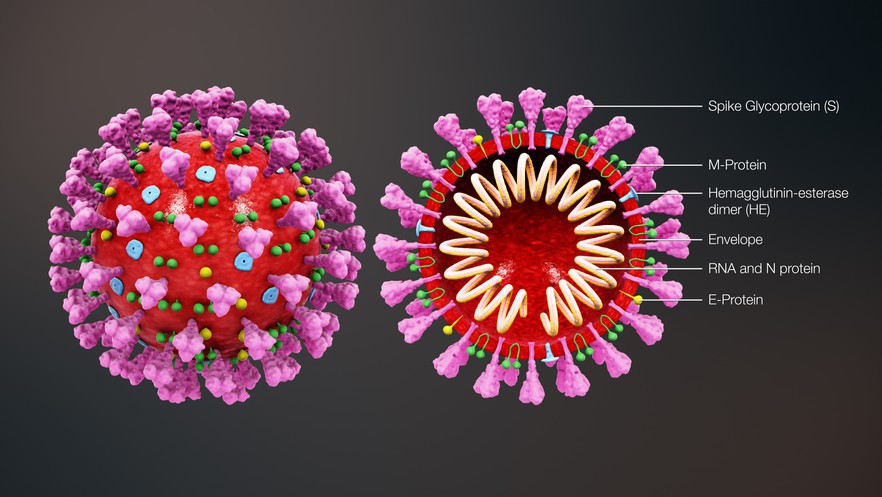
Structure of coronavirus. Image by Scientific Animations via Wikimedia (CC BY-SA 4.0)
28 April 2020
Many journalists, including us, are finding the quantity of science reports on Covid-19 overwhelming. The aim of this occasional column, which we’re calling Covid-19 Report, will be to alert reporters in South Africa (and anyone else who is interested) to the best and most important science, and also clear up misconceptions.
We will draw on the leading peer-reviewed medical and science journals. We’ll also keep a very cautious eye out for good articles published by reputable news organisations and an especially cautious eye on ArXiV, the source of a few good but not yet peer-reviewed science articles. We’re also on the lookout for nonsense, which we’ll debunk.
Covid-19 Report is a joint publication by Spotlight and GroundUp. The people working on it are infectious disease modellers with many years experience reporting the HIV epidemic.
Perhaps the most important development in Covid-19 science this past week has been an article in Science pleading for an end to scientific shortcuts. The authors of Against pandemic research exceptionalism warn that Covid-19 is not an excuse for lowering scientific standards.
“The global outbreak of coronavirus disease 2019 (COVID-19) has seen a deluge of clinical studies, with hundreds registered on clinicaltrials.gov. But a palpable sense of urgency and a lingering concern that ‘in critical situations, large randomized controlled trials are not always feasible or ethical’ perpetuate the perception that, when it comes to the rigors of science, crisis situations demand exceptions to high standards for quality,” the authors write. The authors then describe five standards that research should meet.
An article in Nature makes a related point. Chloroquine hype is derailing the search for coronavirus treatments explains that we may have made more progress answering questions about chloroquine (including hydroxychloroquine) as a treatment for Covid-19 by now “if there had been a rapid, international effort to develop a rigorous chloroquine clinical trial” instead of the “more than 100 clinical trials” that we’re sitting with.
The article points out two more problems with chloroquine hype: it’s hard for non-chloroquine trials to find volunteers (because too many patients insist on being part of a chloroquine one) and the rush on chloroquine stocks means that others who need the drug, such as people with rheumatoid arthritis and lupus, may struggle to get it.
Meanwhile, the Lancet reports that, as of 21 April, “well over 500 clinical trials have been registered at the various international and national clinical trial registry sites”.
To say that’s unprecedented and chaotic for a disease that didn’t have a name until a few months ago is an understatement.
***
How does SARS-CoV-2 (the coronavirus that causes Covid-19) kill? An article in Science, How does coronavirus kill? Clinicians trace a ferocious rampage through the body, from brain to toes, explains how Covid-19 affects all parts of the body. It’s well-written and not too difficult to follow.
***
This article in the NEJM documents how Covid-19 killed 17% of the residents in an American retirement home, or 26% of those infected.
***
How long are people infected with coronavirus before they show symptoms? And when do they become infectious? Research published in AIM found that 50% of people develop symptoms after 5.1 days and 97.5% develop symptoms within 11.5 days. The researchers warn though that their data may be overrepresented by severe cases. (You may have read similar numbers elsewhere, but this is peer-reviewed, methodically carried out research published in a leading medical journal.)
***
This study in JAMA describes the characteristics of 5,700 hospitalised Covid-19 patients in New York. Six in ten of the patients were male. “The most common comorbidities were hypertension (3026, 56.6%), obesity (1737, 41.7%), and diabetes (1808, 33.8%).” 6% had no comorbidities, 6% had one and 88% had more than one.
The HSRC surveyed 19,330 people on the lockdown. Here’s a slideshow and summary. Concerning findings are that a quarter of people surveyed said they did not have enough money to buy food during the lockdown, 13% of people on chronic medications said they could not access them, more than half of people who encountered police said they were treated roughly or rudely by them, and 63% said the lockdown will make it hard to pay their bills. Most people reported complying with the lockdown.
(Note to HSRC: Your website is difficult to navigate. We couldn’t find the full report which is why we linked to one sent to us that we’ve uploaded to our website.)
***
The MRC published an analysis of weekly deaths from 1 January to 14 April. In the period following President Ramaphosa’s announcement of social distancing measures, the actual number of deaths was lower than normally would have been expected over this period. This was because of a “decline in the number of deaths from non-natural causes (eg road traffic fatalities and homicide)”. There is no sign yet of an uptick in natural deaths in people over the age of 60. The MRC intends to publish updated reports every week. These will be worth keeping an eye on since they may in time provide insights on COVID-19-related deaths outside of hospitals.
***
The latest issue of the SAMJ has interesting articles on the ethics and practicalities of who, when and how to quarantine people with Covid-19. One of the articles states: “While limitation of rights may occur in the public interest in the context of a pandemic, it is also important that it does not have the paradoxical effect of increasing spread of infection and public risk. This would be the case if there is fear, intimidation, abuse or victimisation. Under such circumstances the aim of containing the infection will be defeated, as patients avoid testing for fear of what they see as incarceration.” In this regard, watch this court case.