Fewer babies born with HIV in South Africa
Programme changes over last 15 years have yielded excellent results
Fewer than two babies out of every 100 born to HIV-positive mothers in South Africa are infected with HIV at birth. These low rates point to the success of the prevention of mother-to-child transmission (PMTCT) programme in South Africa that has resulted in a decrease of the transmission rate from about 30% at six weeks in the early 2000s, to the 2015/2016 rate of 1.5%.
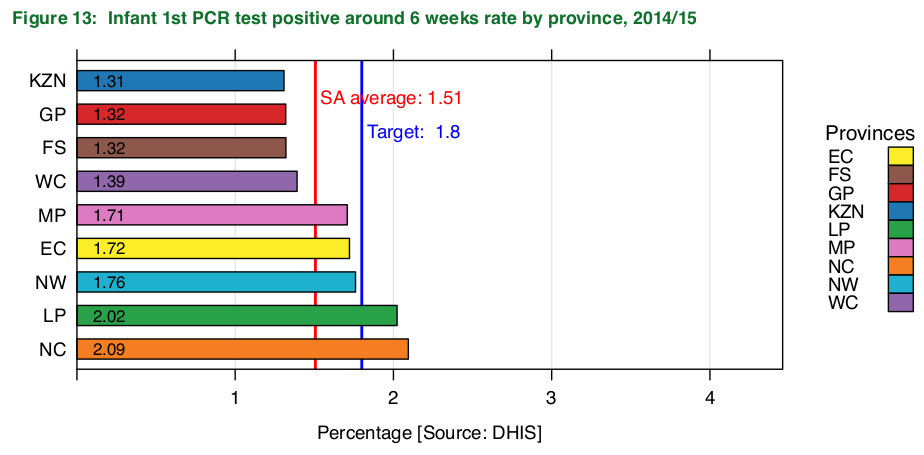
The Western Cape, which pioneered the country’s PMTCT programme in the late 90s and early 2000s, has often been one step ahead. In 2003, the province’s mother-to-child transmission figure was 17.3% at six weeks. In the 2014/2015 year the rate was down to about 1.4% – under the national target of 1.8%. The most recent figures in the Western Cape show that from April to December last year, at ten weeks after birth, the rates of mother-to-child transmission peaked at 1.4% and at their lowest were just over 0.4%.
Neshaan Peton, the Western Cape’s Deputy Director of the HIV Treatment and PMTCT programme, told GroundUp that changes in how the province dealt with mother-to-child transmission have been linked to a drop in transmission rates. “With every policy change a decrease in transmission from mother to baby was noted at six weeks after giving birth,” said Peton.
If a pregnant woman comes into a healthcare facility in the Western Cape, she is tested for HIV and if positive she is initiated on ART on the same day. Peton said that ideally the woman should come into the clinic before 20 weeks. The earlier she comes in, the lower the chances are of transmission to her baby. Babies infected at birth are initiated on antiretroviral treatment. If they do not have HIV at birth, they are tested again at ten weeks.
Babies however can still be infected via breastfeeding. Although antiretroviral treatment prevents breastfeeding mothers from transmitting the virus, if they develop resistance to treatment or are unable to adhere to their medicine regimen, their babies can still become infected. There is however a lack of data on how many infections occur this way, which is why clinicians have called for testing of babies at nine months. (Breast milk, if the mother is on antiretroviral treatment, is a healthier option for babies than formula milk.)
The rest of the country is doing well too. The current makeup of the programme is very different from the first national programme in 2002. That programme was only implemented after the government was ordered to do so by the Constitutional Court. This came after the Treatment Action Campaign (TAC) took the Minister of Health to court to compel her to expand the PMTCT programme nationwide.
Three years before, the first public programme had been rolled out in Khayelitsha, supported by Medécins Sans Frontières. The delay in the rollout of the national PMTCT programme was responsible for “thousands of infant infections and subsequent deaths”.
The Western Cape was also the first province to launch a province-wide PMTCT programme in 2002/2003, reducing rates from 17.6% to 10.3% at six weeks. In 2004, the province began providing two antiretrovirals instead of the single dose that the national programme supplied. In 2005, the rates were down to 6.1% at six weeks. In 2010, co-coordinators were appointed specifically for the PMTCT programme to focus on early booking interventions, postnatal follow up and linkage to care for both the mother and the baby after delivery. Following this change the rates went down from 3.2% to 1.9% at six weeks.
In 2013, the Western Cape implemented what is known in the jargon of the HIV field as option B+: lifelong antiretroviral therapy for all HIV-positive pregnant and breastfeeding mothers irrespective of their CD4 count. (Nationally, this change was implemented in 2015.) In 2016 the province moved to testing all HIV exposed babies at birth. Previously, only high risk babies were tested.
The programme experiences challenges with teenage mothers who can be lost to follow-up and may not adhere to the programme. Neshaan said the programme would also like to improve rates of breastfeeding mothers who return for testing.
Support independent journalism
Donate using Payfast

Don't miss out on the latest news
We respect your privacy, and promise we won't spam you.
Next: Masiphumelele High School fund-raising campaign beats target
Previous: Nairobi sex workers want a research code of conduct
© 2017 GroundUp. 
This article is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
You may republish this article, so long as you credit the authors and GroundUp, and do not change the text. Please include a link back to the original article.

